Mohs Surgery
Mohs micrographic surgery is a safe and highly effective technique whereby skin cancers are removed under complete microscopic control.
In Mohs surgery, a minimal area of skin is removed around the visible cancer. Detailed maps are then drawn of the area, and 100% of the tissue margin is examined under the microscope to be sure all of the cancer and its roots are gone. If any cancer remains, that exact area of involvement is sampled, and the entire process is repeated until the cancer is totally eradicated. This procedure allows physicians trained in Mohs surgery, to see beyond the visible disease, and to precisely identify and remove the entire tumor, leaving healthy tissue intact and unharmed. Mohs surgery minimizes the chance of regrowth and decreases the potential for scarring or disfigurement.
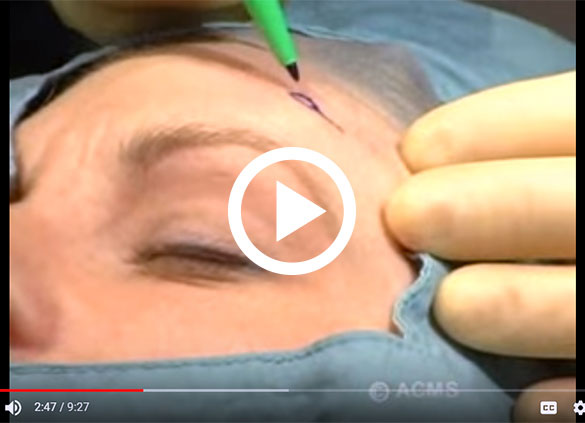
Why Mohs? Skin cancer is the most common cancer in the United States. Watch the video to learn why Mohs surgery is the most effective treatment available. The American College of Mohs Surgery (ACMS) is the only organization that requires its members, after their years of residency training, to successfully complete an extensive fellowship of at least one full year of hands-on training in the Mohs procedure under the supervision of a highly qualified instructor. Learn more by visiting the ACMS Patient Education site.
Click to review the American College of Mohs Surgery (ACMS) Patient Education Video
Indication for Mohs Surgery
Mohs surgery is used primarily to treat basal cell and squamous cell carcinomas, but can also be used to treat less common tumors, including melanoma. Mohs surgery is indicated when:
- The cancer is in a difficult area where it is important to preserve healthy tissue for maximum functional and cosmetic result, such as eyelids, nose, and lips
- The cancer was treated previously and has recurred in the same area
- The cancer is large
- The edges of the cancer cannot be clearly defined with the naked eye
- The cancer grows rapidly or uncontrollably
Advantages to Mohs Surgery
High cure rate – 99% for untreated skin cancers and 95% for recurrent cancers. In Mohs, 100% of the margin is viewed, yielding a higher cure rate. Unlike Mohs surgery, with a routine pathology lab, only a small percentage of the removed tissue is evaluated with 1% of the margins viewed. If cancer cells are present in unexamined sections, they will be missed and the cancer can recur.
Sparing of tissue which offers a better cosmetic outcome. Since the Mohs surgeon is also the pathologist and by using the mapping technique with microscopic control, the mohs surgeon can pinpoint areas involved with cancer that are otherwise invisible to the naked eye. Healthy tissue is spared by taking a minimal margin around the cancer, therefore decreasing the size of the final defect which in turn gives you superior cosmetic outcome.
Tumor Removal in One Day – Because the Mohs procedure is performed in the surgeon’s office and the pathological examination is conducted immediately, the entire process is most often completed in a single day. Unlike Mohs surgery, with standard surgery, the slides are not examined the same day allowing the chance of finding a positive margin at an outside pathology lab and having to perform surgery again at a later date to try and achieve a negative margin.
What to Expect
Please arrive at our office at the specific time assigned to you. This is a surgery appointment and different than a regular office visit. Your actual surgery time will be roughly one hour after you arrive. The physician needs to thoroughly review your case and your surgical suite needs to be prepped. Once the preparation is complete, our staff will escort you into an exam room where Dr. Rausch will discuss your case and further explain the procedure.
A local anesthetic is injected into the skin. Once the area is numb, the cancer and a layer of tissue around it is removed. This part of the procedure takes 10 to 15 minutes. A temporary dressing is applied and you’re escorted to our waiting area. While you wait, the tissue is taken to our lab to be mapped, color coded and examined under the microscope by Dr. Rausch. This part of the procedure takes a minimum of two hours. If any additional affected area is identified, the process is repeated until all of the cancer is removed. The number of stages or layers required depends on the size and depth of the tumor. Since we cannot predict in advance the number of stages necessary to fully remove the tumor, you should plan on spending the whole day with us.
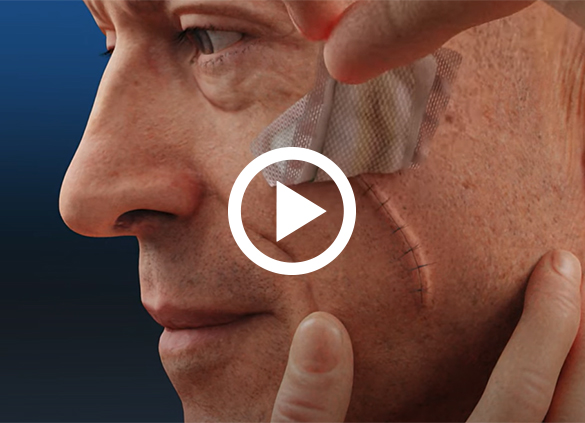
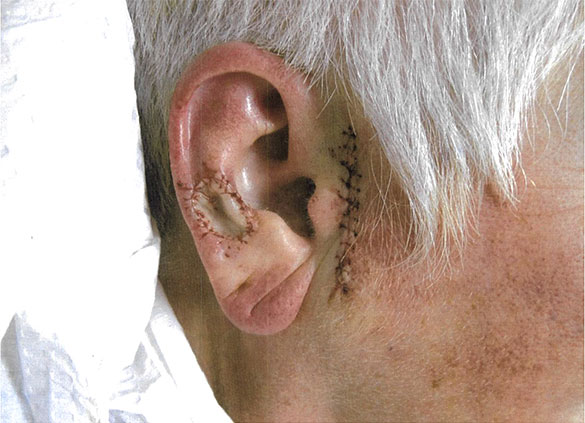
It’s important to realize that Mohs surgery involves cutting the skin, not just scraping. One is left with a hole after the tumor is removed. Options for repair are difficult to determine before surgery since one can not predict the final defect. However, once the area is cancer free, Dr. Rausch will discuss the options for wound healing and surgical repair of the defect. They include letting the wound heal by itself, closing the wound in a side-to-side fashion with stitches, or closing the wound with a skin flap or graft. Repairing locations on the nose, ear, eyelid or lip can often be more involved than anticipated because these locations do not have tissue that can be brought together easily. Filling the hole can be more of a challenge, often requiring a flap or graft. Following the repair, a dressing is applied and you will be given instructions on wound care and dressing changes. Occasionally, if warranted, other surgical specialties may be utilized for their unique skills.
Pre-operative Consultation: Consultations with Dr. Rausch are done the day of surgery but can be arranged prior to surgery if desired. If you’re uncertain about surgery because you are considering another form of treatment or no treatment at all, please call before your scheduled surgery date to avoid a cancellation fee.
Biopsy Site Identification: Smaller cancers are difficult to identify. You must be able to identify your biopsy site the day of surgery. It’s helpful to take a photo of your biopsy site before it heals. Bring the photo with you the day of surgery or email to info@mohsvirginia.com (photos you send may not be encrypted).
Medications:
Continue all medications, except narcotics and benzodiazepines, prescribed by your doctor, including blood thinners, aspirin, Coumadin, Plavix, Vitamin E and blood pressure medications. Studies show discontinuation of prescribed medications, even for short periods, can put one at risk for life threatening events, such as heart attack and stroke.
Do NOT take any benzodiazepines- Diazepam (Valium), Lorazepam (Ativan), Alprazolam (Xanax), Clonazepam (Klonopin), Temazepam (Restoril), Chlordiazepoxide (Librium), Clorazepate (Tranxene), Oxazepam (Serax), or narcotics- Codeine, Fentanyl, Hydrocodone, Lortab, Norco, Vicodin, Hydromorphone (Dilaudid), Demerol, Methadone, Morphine, Oxycodone, OxyContin, or Percocet the day of your surgery. Identification of the site and signing of the consent form need to be done PRIOR to taking any of these medications. Bring your medication with you the day of surgery, and it can be taken after signing the consent. If any of these medications are taken prior to signing the consent, surgery will be canceled and a cancellation fee will apply.
Food and Drink: Since surgery is performed under local anesthesia, you may eat and drink that day. We recommend bringing a lunch with you. Our coffee bar has a refrigerator and microwave available for your use. You will be asked to remain in the office during the procedure, but your companion can visit one of the eateries located near our office and bring you back lunch or a snack.
Alcohol: Alcohol promotes bleeding. We ask you to avoid alcoholic beverages 48 hours before/after surgery.
Smoking: Smoking can affect healing by diminishing blood supply at your surgery site. Discontinue smoking 2 days before surgery and for 1 week after surgery. If you can’t discontinue entirely, cut back to less than 1 pack per day.
Transportation: Make arrangements for someone to drive you the day of surgery. Patients given medicine to relieve anxiety will not be allowed to drive themselves home.
Attire: Wear comfortable, older clothes, avoid make-up, perfume and jewelry. If surgery is on an area covered by clothing, wear something easy to remove.
Passing Time: Bring reading material or your computer to occupy time while waiting for the microscope slides to be examined. Wireless internet access is available.
Cancellations: If you must cancel surgery, please cancel 48 business hours before your surgery date. Less than 48 business hours notice will result in a cancellation fee.
[VIDEO] Postoperative Care for Mohs Surgery
Please don’t travel outside the area for 1 week so that any post-operative issues can be addressed. If you have any problems at home after surgery, please do not hesitate to call our office. Verbal and written instructions for wound care will be given to you at the end of your day.
Will I have pain and bruising after surgery? The surgical site may be sore for several days. Tylenol and Ibuprofen are usually adequate for relief. Bruising and swelling are common and may not peak until 48 hours after surgery. Do not plan surgery around an event where your physical appearance is important as you’ll be wearing a bandage for a week in most cases.
Will I be able to return to work or be able to drive? If you’re given medications during surgery, you will not be allowed to drive yourself home. Returning to work or driving will depend on the size and location of your cancer/abnormal lesion and your occupation. Please bring all FMLA paperwork with you the day of surgery. In most cases, time of work will not be granted after surgery. Specific restrictions will be discussed the day of surgery. If
you would like to discuss this prior to surgery so arrangements can be made ahead of time, a consult is required.
Can I exercise after surgery? Activities, including exercise or heavy lifting, will be restricted until stitches are removed. The more activity you participate in, the more likely you may bleed from the surgery site.
Will the surgery leave a scar? Whenever surgery is performed, there will be a scar. Dr. Rausch is trained in advanced reconstruction and fine suturing techniques to optimize the cosmetic outcome.
Will I need to come back? Suture removal and wound evaluation are usually performed one week after reconstructive surgery, which will not be done until the pathologist determines that all the cancer is removed. In some cases, visits may be needed over the next several weeks to months. Periodic visits at least once a year to your referring physician are advisable to monitor for skin cancers or signs of recurrence.
What causes skin cancer? The most important factor in the development of skin cancer is sun exposure.
Why should skin cancers be treated? The two most common types of skin cancer are basal cell and squamous cell carcinoma. Basal cell carcinomas grow slowly and rarely spread throughout the body, but can be locally destructive if not removed entirely. Squamous cell carcinomas can spread to lymph nodes and other parts of the body.
What treatments are used for skin cancer? Methods include curettage (scraping the tissue), excision (cutting the tumor out), radiation therapy, topical cream, and Mohs micrographic surgery. The treatment modality is based on several characteristics of the skin cancer, including location, size, aggressiveness and recurrence. Your physician is knowledgeable of the various treatment.
How can I protect myself in the future? Early detection is critical. Studies show that people who perform skin self exams have thinner, less advanced melanomas. Early detection can reduce mortality by 63%. Regular skin exams by your physician are essential. Minimize your sun exposure and avoid tanning beds -- studies show a 75% increase in melanoma risk when indoor tanning began before age 30.